SouthCare Animal Medical Center
Category:

Lilies – Toxic to our feline friends!
General
Lilies are beautiful plants which may brighten your home, but they are highly toxic to your cat.

Stool Eating: Your Dog’s Dirty Little Secret
General
It’s the stuff of which nightmares are made. Your best pal, Ringo, the greatest dog in the world, so clever, so cute, looks up, tail wagging with a self-satisfied expression, and then you notice—he’s snacking on cat droppings stolen from their litter or other droppings from outside! Oh no! That’s disgusting! How could you!? You’re remembering the last time he licked your face… than start to feel queasy.

The New Coronavirus and Companion Animals
General
Coronaviruses belong to the family Coronaviridae. Alpha- and beta-coronaviruses usually infect mammals, while gamma and delta coronaviruses usually infect birds and fish. Canine coronavirus, which can cause mild diarrhea and feline coronavirus, which can cause feline infectious peritonitis (FIP), are both alpha-coronaviruses. These coronaviruses are not associated with the current coronavirus outbreak.

Cancer in Pets – The Warning Signs
General
Lumps, bumps, growths, and swellings are signs indicative of health issues that could be potentially life-threatening. As our pets continue to live longer lives, it is imperative that any symptom of a tumor be examined by a veterinarian.

Four Steps to Help Fido’s Anxiety
General
No matter how much we love our dog, leaving the house and the dog home alone is a part of life as a pet owner. For some dogs, this can cause anxiety and stress, resulting in mild to severe separation anxiety. Some breeds are more prone to it, and life changes, like a move to a new house or the loss of an important person, can cause it. It’s important to remember some of the symptoms of separation anxiety are similar to other behavioral conditions, such as a dog that is not fully house-trained. If you suspect your dog is suffering from anxiety, monitor and record his behavior patterns to discuss them with your veterinarian.

When should you take your pet to the vet for eye problems?
General
Is your dog pawing at its eye? Does it have a green discharge? Is your cat’s eye bulging?
Sometimes, it’s difficult to determine when a condition is serious enough to take your pet to the veterinarian.
However, when it comes to eyes, even minor symptoms can be signals of serious eye disease.

Do you know the signs of ear infections?
General
The ear canal is the tubular portion of the outer ear that carries sound to the tympanic membrane (eardrum). The most common disorder of the ear canal is otitis externa. Routine (at home) examination and cleaning of your dogs’ ear canal is essential for its overall health, especially if it is a breed predisposed to inflammation of the ear canal.
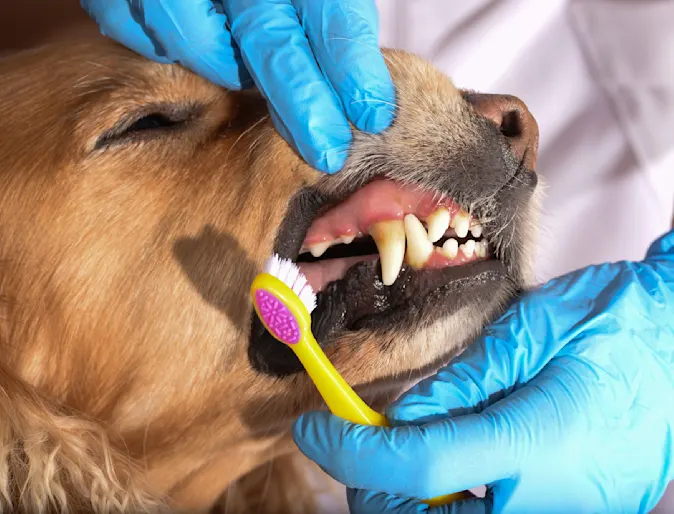
Dispelling Pet Dental Myths
General
Did you know that approximately 80% of adult dogs and 70% of adult cats have some form of oral disease? Dental problems are among the top three pet owner concerns in dogs and cats. There are many misconceptions about how to provide good oral care to your pets. Here is a list of the most common myths that people believe about their pets dental health.
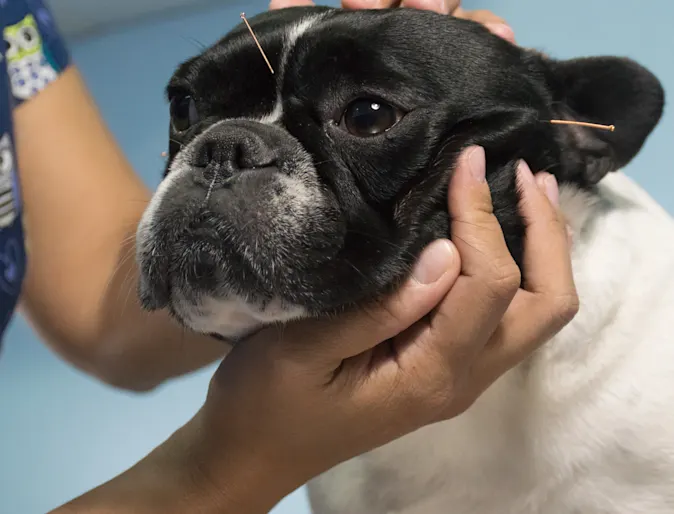
Can Acupuncture Help My Pet?
General
Some of you may have already asked yourself this question, or maybe even wondered if acupuncture is a valid treatment option. I mean, it’s a little out there, right? Does it actually help? Hopefully the following post will help answer some of these questions, and give you the information you need to decide if acupuncture would fit into your pet’s already established treatment regimen.

Getting Skunk spray off your pets
General
Oh, no! Max has been skunked! You know what has happened long before Max made it into the house. It’s that super strong smell that can’t be ignored- skunk spray! Poor Max was having such a great time…. right until he wasn’t.

Black Fly Bites vs. Target Lesions
General
Its officially black fly season and these are unavoidable nuisances in some parts of the Spokane area. Black flies may not only find you a tasty feast, but also your pet.

Spring & Tick Season
General
It’s only a few more weeks until spring! Our days are getting longer and we even have the equinox countdown going at SouthCare. We are so excited for our beautiful Spokane spring!

When Pets Encounter Porcupines
General
Porcupines are the 3rd largest rodent in America, second only to the beaver. Porcupines can be active during the day or night.